Abstract
Aging brings additional challenges in the management of people with von Willebrand Disease (VWD). Plasma von Willebrand Factor (VWF) levels may increase but the impact on bleeding phenotype is unclear. With the development of age-related comorbidities, the use of antiplatelet (AP) or anticoagulant (AC) therapies may be warranted. As highlighted in the 2021 international VWD guidelines, limited evidence exists regarding the bleeding risk and safety of AP/AC use in people with VWD. 1 We sought to address this knowledge gap through a retrospective review of a large cohort of people with VWD attending a tertiary referral center.
The records of all patients aged >50 years (y) attending our center registered with VWD were retrospectively reviewed. We identified all individuals treated with AP and/or AC, recording the indication for and duration of therapy. We also recorded disease subtype, baseline and most recent plasma VWF levels and bleeding on AP and/or AC. Bleeding episodes were stratified according to the World Health Organization (WHO) Bleeding Scale.
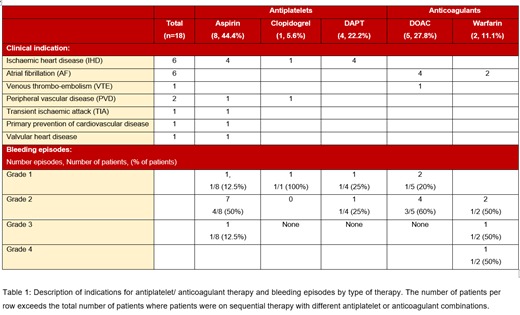
From 255 eligible patients, 18 patients (7 male, 11 female) were identified who received AP and/or AC over a period of 22y. The median age at commencement was 60.2 years (range 40.0-74.5). 15 patients had Type 1 with baseline levels 30-50 IU/dL, (median VWF antigen, VWF:Ag, 57.5, range 39-87 IU/dL; median VWF ristocetin cofactor levels, VWF:RCo, 43, range 35-54 IU/dL). 3 patients had type 2 VWD (median VWF:Ag 64, range 27-90 IU/dL; median VWF:RCo of 16, range 10-66 IU/dL). The type of AP/AC used and indications for treatment are outlined in Table 1.
Overall, 12 patients were treated with AP and 7 with AC therapy (19 therapies in total as one patient received first aspirin then warfarin therapy). The cumulative exposure to AP therapy was 61.9y with a median exposure time of 3.2y/patient (range 0.3-14.1y). Duration of AC therapy was shorter, with a cumulative exposure of 17.6y and a median of 1.5 y/patient (range 0.3-6.3y).
Overall, 85.7% of patients on AC therapy had at least one episode of bleeding (6/7; 10 episodes total) in contrast to 58.3% of patients on AP (7/12; 12 episodes total). Of these 22 episodes, 5 (22.7%) were grade 1 bleeding. Grade 2 bleeding (iron deficiency or gastrointestinal (GI), gynecological or genitourinary bleeding) occurred in 5 patients (41.7%) treated with AP and 4 patients (57.1%) on AC (total of 14 episodes). 1 episode of grade 3 bleeding occurred in both the AP (8.3%) and AC (14.3%) group (GI bleeding requiring transfusion and abdominal hematoma respectively). The single grade 4 bleed was an intracranial hemorrhage (ICH) and occurred in a patient with type 2 VWD (VWF:RCo 10 IU/dL) on warfarin for atrial fibrillation; this required prothrombin complex concentrate, VWF concentrate, neurosurgical intervention and cessation of AC.
Bleeding complications resulted in discontinuation of therapy in 2 patients (11.1%) treated; the individual with ICH and a patient with type 1 VWD on warfarin (baseline VWF:RCo 43 IU/dL) due to recurrent GI bleeding. No patients treated with AP therapy required discontinuation of use. The overall rate of major bleeding (WHO grade >/=3) in our study was 11.4 events/100 patient-years in VWD patients receiving AC therapy, in comparison to the rate of bleeding in the general population using AC of 7.2 events per 100 patient-years. 2
For patients with type 1 VWD, plasma VWF levels were seen to increase during follow up (median 8.5y, VWF:Ag median +13 IU/dL, VWF:RCo +18 IU/dL), resulting in plasma VWF levels >50 IU/dL for 66.6% of patients in this cohort. Despite this, bleeding while on AP and/or AC was still experienced in 8/10 patients whose levels had normalized, necessitating cessation in one instance.
In conclusion, this study provides important insights into the use of AP and/or AC in patients with VWD. Bleeding rates were higher in patients treated with AC therapy than AP resulting in cessation of therapy in 28.6% of those on AC. Bleeding events still occurred despite normalization of plasma VWF levels in patients with type 1 VWD. These data highlight the need for close follow up of patients with VWD whilst on antithrombotic therapy, particularly AC.
1. Connell NT et al. ASH ISTH NHF WFH 2021 guidelines on the management of von Willebrand disease. Blood Adv 2021;5(1):301-325.
2. Shoeb M, Fang M. Assessing Bleeding Risk in Patients Taking Anticoagulants. J Thromb Thrombolysis 2013;35(3):312-319.
No relevant conflicts of interest to declare.
Author notes
 This icon denotes a clinically relevant abstract
This icon denotes a clinically relevant abstract